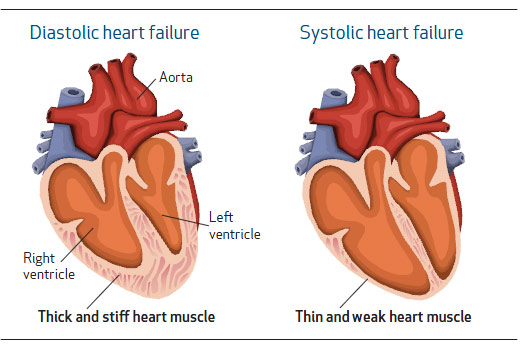
 Congestive heart failure (CHF) traditionally has been thought to be the result of impairment in the heart’s ability to contract and expel blood, a condition called systolic heart failure. However, it is now recognized that 50 percent of patients with heart failure have an abnormality in the relaxation function of the heart that is known as diastolic heart failure. Either form of heart failure—systolic or diastolic— may produce shortness of breath called cardiac dyspnea. Because diastolic heart failure is not as well recognized as systolic and occurs with other common medical problems causing dyspnea, it’s often missed in diagnosis and treatment.
Congestive heart failure (CHF) traditionally has been thought to be the result of impairment in the heart’s ability to contract and expel blood, a condition called systolic heart failure. However, it is now recognized that 50 percent of patients with heart failure have an abnormality in the relaxation function of the heart that is known as diastolic heart failure. Either form of heart failure—systolic or diastolic— may produce shortness of breath called cardiac dyspnea. Because diastolic heart failure is not as well recognized as systolic and occurs with other common medical problems causing dyspnea, it’s often missed in diagnosis and treatment.
In an effort to address the specific needs of patients with dyspnea resulting from diastolic dysfunction, Washington University School of Medicine and Barnes-Jewish Hospital have recently opened the Cardiac Dyspnea Center, one of just a handful of cardiologistrun dyspnea centers in the United States. The new center is part of the Washington University and Barnes-Jewish Heart & Vascular Center.
Headed by Susan Joseph, MD, a Washington University cardiologist specializing in the treatment of heart failure, the new center offers its patients a multidisciplinary treatment plan that covers cardiac and pulmonary issues. In addition to Joseph, patients treated at the center may see Ari Cedars, MD, an expert in exercise physiology and diagnostic heart catheterization, and VictorDavila-Roman, MD, a specialist in echocardiography and other noninvasive testing. Patients also are always seen by Washington University pulmonologist Stephen Lefrak, MD, because other causes of dyspnea frequently co-exist with cardiac dysfunction and must be ruled out or appropriately treated.
“In addition to cardiac dysfunction, dyspnea patients often have many conditions that cloud the diagnosis. Most of them have a high body mass index, sleep apnea or an underlying lung disease; those things alone can change respiratory function,” Lefrak says.
On the cardiac side, Joseph says that often primary care physicians don’t realize that the shortness of breath their patients are experiencing is due to heart failure. This is because on typical heart imaging, the squeezing, or systolic, function of the heart is normal. One characteristic of cardiac dyspnea is increased pressure in the heart during the heart’s period of relaxation, or diastole, something that can be detected during a right heart catheterization.
“Normally, the pressure inside the left ventricle between beats is low. In people with other health problems such as obesity, diabetes, hypertension and coronary artery disease, the ventricle becomes stiff and can’t relax,” Joseph says. “The pressure at rest may be elevated. These high pressures lead to shortness of breath and fluid accumulation in the lungs, which together characterize congestiveheart failure.”
Joseph explains that diastolic heart failure patients may be fine at rest, but with exertion, may become short of breath due to increased pressure in the heart, even without retaining extra fluid.
Each new patient seen at the dyspnea center does a six-minute diagnostic walk under the careful guidance of clinic coordinator Anne Renick, RN. During the test, she is able to gather information on the distance traveled, heart rate, blood pressure and oxygen needs to add to other diagnostic information. The results of this test help the center’s physicians treat the whole patient, including any conditions that complicate the cardiac issues.