The patient lies on his side on the operating table, alert and chatting with the anesthesiology team about his love for St. Louis Blues hockey and reality shows, and about which team he favors in the upcoming Super Bowl.
Washington University neurosurgeon Eric Leuthardt, MD, interrupts.
“Tim, how are you doing?” he asks.
“Great,” the patient says wryly. “Just living the dream.”
“Glad to see you have your sense of humor,” Leuthardt replies, as he returns to the task at hand: tweezing strands of tumor tissue from the patient’s exposed brain.
The patient is one of about 15 patients a year who undergo awake craniotomy surgery performed by Washington University neurosurgeons at Barnes- Jewish Hospital. Though it may seem shocking to wake a patient in the middle of surgery—especially a major surgery on a vital organ—awake craniotomy is a valuable treatment for brain tumors and intractable seizures in carefully selected patients.
“With awake craniotomy, patients derive better outcomes,” says Leuthardt, director of the Center for Innovation in Neuroscience and Technology, Department of Neurological Surgery. “We’re able to accomplish a more aggressive surgery in sensitive areas while preserving function.”
In a standard open craniotomy, part of the patient’s skull is removed so surgeons can access the brain. It’s a common procedure for removing many brain tumors, repairing acute brain hemorrhages or trauma and removing clots or tissue causing seizures. Patients remain fully anesthetized—asleep—during these procedures.
The difference with awake craniotomy is that after the patient’s skull is opened and before surgeons begin cutting or manipulating brain tissue, the patient is brought out of sedation to consciousness in order to interact with the surgical team.
Awake craniotomies are primarily performed on patients who have lesions near the areas of the brain that control speech and motor function.
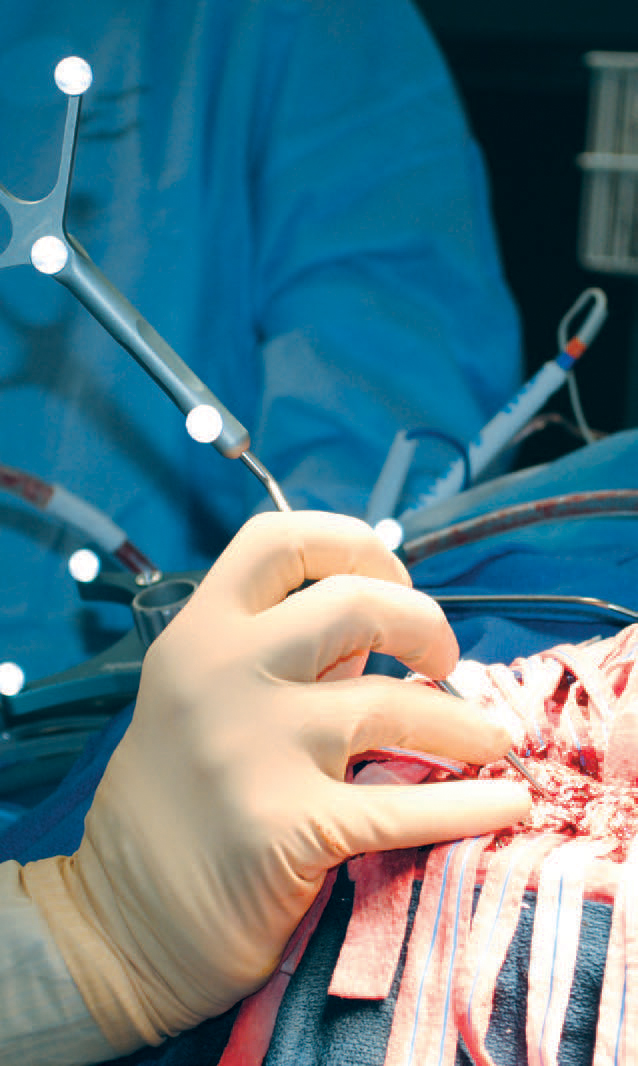
Eric Leuthardt, MD, uses a special probe to check his exact position within the patient’s brain.
|
While removing or destroying troublesome tissue, surgeons need to ensure that they’re not inadvertently damaging healthy tissue. The most reliable way to do this is to wake the patient up, ask him or her to answer questions and perform simple tasks, and then monitor the responses.
“This procedure can give the surgeon the best balance between safely avoiding critical areas in the brain while at the same time being maximally aggressive towards the tumor,” Leuthardt says.
At Barnes-Jewish Hospital, several advanced technologies are available to supplement this technique, making awake craniotomy even safer and more precise.
For instance, awake craniotomies are performed in the hospital’s intraoperative magnetic resonance imaging (MRI) suite.
This suite is one of about 20 in the United States equipped with a high-field-strength MRI magnet, which allows surgeons to produce real-time MRI scans during surgery. Surgeons can then consult the images to make sure they’ve removed as much tumor tissue as safely possible.
Washington University neurosurgeons also use stereotactic navigation, a system that works like a GPS to guide them through the patient’s brain.
The day before surgery, the patient has an MRI to map certain points in the brain. The map is displayed on a screen during the operation, and surgeons check their exact position within the brain by touching the area with a special probe.
Leuthardt also uses sophisticated brain-mapping techniques, some of which he developed, to pinpoint areas of the brain that control very specific behaviors.
One technique involves laying a thin plastic sheet studded with a grid of sensors directly on the brain’s surface. The sensors detect minute electrical charges as they travel along pathways in the brain during a seizure or while the patient is speaking or moving.
A computer program turns the data collected by the sensors into a map that can guide surgeons precisely to the area causing seizures or steer them away from healthy tissue surrounding a tumor. But sophisticated technology is ultimately just a complement to the skill and experience the surgical team must bring to the procedure. The volume of awake craniotomies performed at a center translates into better outcomes, and the Washington University neurosurgeons are experienced at surgery close to the motor and sensory cortexes.
Providing anesthesia for awake craniotomies also presents a special challenge, says Leuthardt. Typically, a patient who is asleep during surgery has a breathing tube inserted to keep the airway clear and open. A patient who is awake and talking can’t be intubated, so the anesthesia team must be especially vigilant.
And although the brain itself has no pain receptors, the patient must be kept as calm and pain-free as possible during the surgery, especially as the scalp is cut and a portion of skull is removed. However, the patient can’t be so sedated that he or she can’t respond to the surgeon.
“It’s certainly more difficult than a regular procedure,” Leuthardt says.
But awake craniotomy can pay off in both short-term and long-term benefits for the patient.
In the long run, patients with difficult brain tumors can have an extended and improved quality of life when the maximum amount of tumor is removed. In the short run, patients often spend less time recovering in the hospital.
The day after his surgery, the Blues-loving patient is alert and sitting up in the Barnes-Jewish neuro-intensive care unit. He’s drinking a milkshake and talking with his family when Leuthardt stops by.
“Still doing OK?” Leuthardt asks.
The patient flashes a smile and gives his doctor a thumbs up.
Refining the Technique
To remove a tumor near important brain regions governing speech or motor control, neurosurgeons must first identify these areas and map their locations. For half a century, this mapping has been performed by directly stimulating brain tissue with one bipolar electrode while the patient is awake, talking and performing tasks.
According to Eric Leuthardt, MD, director of the Center for Innovation in Neuroscience and Technology, Department of Neurological Surgery, this direct stimulation technique is considered the gold standard for mapping and monitoring brain function during this type of procedure, known as awake craniotomy. “The electrode temporarily stuns a little area of the brain, so you can see what would happen if you were to remove it,” Leuthardt says. “If the patient stops talking, or if he stops moving or jerks his hand, you can identify the areas that control motor and speech.”
Leuthardt calls the technique useful but not perfect.
“It’s inefficient and cumbersome, and it carries the risk of causing seizures,” he says. “So we’ve been developing a number of new techniques to identify brain function, both before and during surgery.” Before the patient enters the operating room, Leuthardt and other neurosurgeons can perform a type of MRI scan that maps the locations of the brain’s networks in a resting state.
Unlike task-based MRI mapping, the patient does not need to actively participate in the testing. The MRI scan maps the resting brain before surgery, and Leuthardt has another tool to map networks during the surgical procedure. With an electrode array that sits on the surface of the exposed brain, he can passively record electrical signals from different parts of the brain while the patient is under anesthesia.
Ultimately, one goal of these new technologies is to limit the need for awake craniotomy. Though Leuthardt says an awake procedure provides the best method to eliminate the tumor while protecting healthy brain tissue, it’s still a lot for patients to go through.
“It’s stressful for people to be awake during these surgeries,” he says. “Now, we can listen to the brain do its thing without passing electricity into it. As a result, we have a good idea of what’s where before they even wake up in the OR. I still do the gold standard—awake stimulation— but these additional capabilities have the potential to make awake brain mapping safer and more efficient.”
To learn more, and watch a video of an awake craniotomy, visit BarnesJewish.org/awake.