Heart disease is common, affecting millions of adults and causing 26 percent of deaths annually. Yet there’s another silent killer lurking nearby that often goes unnoticed and untreated until it’s too late.
Carotid artery disease (CAD) is a serious vascular condition that shows no symptoms in 70 percent of individuals evaluated. It is also a leading cause of strokes.
The carotid arteries, the main source of blood flow to the brain and face, are located on each side of the neck and extend from the aorta in the chest to the base of the skull. A healthy artery is open and allows the blood to flow to the brain efficiently. Blood flow can become partially or totally blocked by fatty material called plaque. As more plaque forms, the artery becomes narrower and the walls become irregular, which can cause blood clots to form on the plaque.
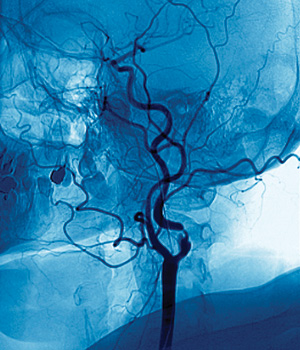 “Carotid artery disease is prevalent in many people, especially those who also have peripheral vascular or coronary heart disease,” says Luis Sanchez, MD, Washington University vascular surgeon at Barnes-Jewish Hospital. “If someone has signs of another vascular condition, doctors often look for CAD to prevent more serious conditions.”
“Carotid artery disease is prevalent in many people, especially those who also have peripheral vascular or coronary heart disease,” says Luis Sanchez, MD, Washington University vascular surgeon at Barnes-Jewish Hospital. “If someone has signs of another vascular condition, doctors often look for CAD to prevent more serious conditions.”
A partial blockage or narrowing of the artery is called carotid artery stenosis. Blockage can reduce the blood supply to the brain and lead to a stroke. A stroke can also result from an embolism, a blockage caused when a clot breaks loose and travels to the brain. If a small blood vessel is blocked, this causes a mini-stroke (transient ischemic attack, or TIA) and is often a warning sign that a larger stroke may soon occur.
As the degree of narrowing increases, so do the risks of stroke and embolization. Patients with high blood pressure, diabetes and high cholesterol are at risk, as are patients who are overweight or smoke.
“There is often a noise in the neck on a routine test or something small that makes us then test for CAD,” Sanchez says. “If symptoms do arise, patients may have a small mini-stroke due to a carotid lesion. A TIA patient can have speaking difficulties, numbness in the extremities, weakness or vision problems. Any or
all of the symptoms can either last just a few seconds or repeatedly for many minutes, so some patients don’t realize the seriousness.”
Not all patients need surgery right away. Drug therapies are often the first line of defense. More serious treatment for carotid stenosis is needed in patients who have had a prior stroke, prior TIA, or severely blocked carotid arteries. Once the diagnosis of significant carotid stenosis is made, meaning there is a 70 percent blockage of the artery, the most appropriate therapy is vascular surgery. This can be one of two procedures, the more common carotid endarterectomy or the newer carotid artery stenting.
Washington University heart and vascular surgeons offer both options with great success.
Carotid Angioplasty and Stenting (CAS)
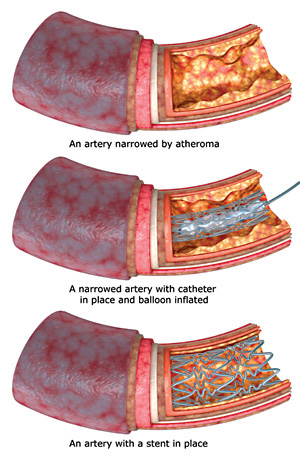 In the past 15 years, surgeons have developed a minimally invasive stenting procedure to combat severe CAD. In the procedure, the surgeon introduces a needle into the artery in the groin after injecting numbing medicine. A catheter, a flexible plastic tube, is inserted into the artery and carefully guided up to the neck where the carotid artery blockage is located. Live X-rays, called fluoroscopy, are taken to see the artery during the procedure.
In the past 15 years, surgeons have developed a minimally invasive stenting procedure to combat severe CAD. In the procedure, the surgeon introduces a needle into the artery in the groin after injecting numbing medicine. A catheter, a flexible plastic tube, is inserted into the artery and carefully guided up to the neck where the carotid artery blockage is located. Live X-rays, called fluoroscopy, are taken to see the artery during the procedure.
The surgeon then passes a guidewire through the catheter to the blockage. Once a filter is placed above the blockage to prevent pieces of plaque from breaking off and causing a stroke, a small balloon at the end of the wire is then inflated and pressed against the inside walls of the artery to open the artery and allow better blood flow to the brain.
Finally, a wire mesh stent is placed across the blocked area. The stent is inserted to help keep the artery open after balloon treatment.
Because the procedure is still new, stenting is more commonly preformed when patients are at high risk, are symptomatic, or have had previous surgeries in the area. It is beneficial, however, because patients are treated under local anesthesia while awake. Staying awake allows the surgeon to monitor the brain’s reaction to decreased blood flow. Patients are usually treated on an outpatient basis and only held overnight for surveillance on the medication.
“Outcomes at Barnes-Jewish are the same as those with the more traditional surgery, and it is the best option for the most severe cases,” says Gregorio Sicard, MD, vice chair for the department of surgery.
“Stenting can be better for patients because there are no pulmonary complications and it puts less stress on the body overall,”
Carotid Endarterectomy
The more traditional procedure is carotid endarterectomy, performed in 90 percent of patients with significant stenosis. Surgeons at Barnes-Jewish Hospital do this procedure 200-250 times per year, one of the highest rates in the country.
To begin surgery, an incision along the side of the neck is made to locate the carotid artery. The surgeon opens the artery, removes the plaque and closes the artery with a patch. This procedure may be done with the patient asleep or under local anesthesia.
Endarterectomy takes about two hours to perform and patients also stay in the hospital overnight for observation. Temporary nerve injury, leading to hoarseness, difficulty swallowing, or facial numbness, can occur and typically resolves within one month without further treatment.
Washington University heart and vascular surgeons participate in clinical trials to assess the effectiveness of carotid endarterectomy and carotid stenting. Sicard helped found the Society for Vascular Surgery-sponsored Vascular Registry, which maintains patient records in order to measure new treatments and also allows surgeons to follow long-term outcomes data on patients who undergo either procedure.
Worldwide, Washington University surgeons provide the largest number of cases to the registry and have among the best short- and long-term outcomes for carotid endarterectomy and stenting.