When Emily arrived at Barnes-Jewish Hospital on the morning of June 14 for her kidney transplant, she was in end-stage renal failure. The kidney that had been doing important work—removing excess water and waste from her blood, transforming poisonous waste products into urine and returning cleansed blood for use throughout her body—was no longer functioning. A dialysis machine performed this role for her before she and a team of specialists determined a kidney transplant would restore a better quality of health and life.
 In the weeks and months leading up to her transplant, Emily is rigorously evaluated by the kidney transplant team. Transplant candidates are assessed for physical, anatomic and psychosocial fitness. They undergo a series of blood and radiology tests. They also meet with dietitians, social workers and finance specialists who are experts in helping patients access available resources. The goal in all this is to ensure a patient has the medical support and determination to withstand both transplant surgery and the demanding postoperative regimen.
In the weeks and months leading up to her transplant, Emily is rigorously evaluated by the kidney transplant team. Transplant candidates are assessed for physical, anatomic and psychosocial fitness. They undergo a series of blood and radiology tests. They also meet with dietitians, social workers and finance specialists who are experts in helping patients access available resources. The goal in all this is to ensure a patient has the medical support and determination to withstand both transplant surgery and the demanding postoperative regimen.
Emily arrives at Barnes-Jewish Hospital with her parents, in-laws, two girlfriends (who keep Emily’s many well-wishers updated via Facebook and Twitter throughout the day) and her husband. Her new kidney, from a living donor, is on an airplane, flying in from New York.
Surendra Shenoy, MD, PhD, a Washington University transplant surgeon at Barnes-Jewish Hospital and director of the living-donor transplant program, is Emily’s surgeon.
The following is a timeline of Emily’s surgery.
14:09:51
Once the plane carrying the donor kidney nears the airport, Emily is assigned a preoperative room. She meets with nurses and anesthesiologists who keep her and her family informed.
Finally, sedation is started and Emily is wheeled to the operating room by the anesthesiology team.
15:07:38
Tracked by GPS as it makes its way across the country, the donor kidney arrives in the operating room and unpacking begins. Prior to the kidney’s arrival, the surgeon who removed the kidney from the living donor discussed with Shenoy the condition of the kidney, any anomalies that could affect transplantation and other relevant information. For instance, the donor kidney Emily receives has two arteries instead of one. Differences of this kind are not unusual.
15:11:45
Upon the patient’s arrival in the operating room, her abdominal cavity is prepared to receive the donated kidney. Unless the failed kidneys are causing infection or high blood pressure, they are left in place. The new kidney will be located in a space created for it within the abdominal cavity.
15:11:47
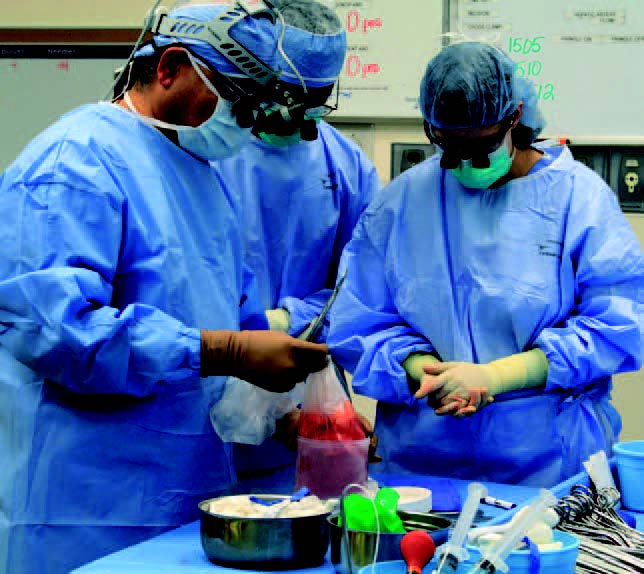
The donor kidney is removed from its packing materials to an area within the operating room where it will be prepared for transplantation. The preparation process is called benching the kidney. It is this process that ensures the kidney remains healthy and viable up to the moment it is sutured in place in the recipient.
15:35:27
Because a kidney can survive for just five to 10 minutes without blood flow once it’s removed from the body, it is kept cool in a slush of ice to preserve the exterior. The interior is maintained with injections of a cold solution of preservatives designed to keep cells alive despite the lack of blood flow. In this manner, a kidney can be kept viable for 24 to 48 hours.
“A kidney from a live donor is more likely to endure this preservation process than one from a deceased donor,” says Shenoy.
 15:45:27
15:45:27
Shenoy and his surgical team arrange the kidney in the prepared abdominal cavity, checking several times for optimal placement. Once the best orientation for placement is determined, the kidney is returned to its bath of slush, and the abdominal cavity is further prepared.
“A transplant surgeon must tailor the implantation to the anatomy of the donor organ and the recipient,” says Shenoy.
16:37:10
The kidney is removed from the preservative and placed in the abdominal cavity in proper orientation.
“In this case, the kidney has two arteries, one of which is situated in an unusual position.”
17: 11:56
With the kidney in place, Shenoy and his team begin to connect the organ’s veins and arteries to the patient’s blood vessels and the ureter to the patient’s bladder.
“The kidney must be situated so that there are no kinks or twists in the connections that may impact its function.”
17:45:37
When first placed in the body, the kidney is pale pink. Once the arteries are connected and blood begins to flow into the kidney, it becomes a more vivid color.
18:22:00
“It’s a delicate job to join a tube that is 3 to 4 millimeters in diameter to another of similar size. The sutures are made with thread as thin as a hair.”
19:07:35
Now placed within the abdominal cavity with the ureter, veins and arteries connected, the kidney begins to work. When a healthy kidney makes urine, the bladder can hold 300 to 400 milliliters—up to one-half liter of urine at a time. If a bladder is connected to a failed kidney that does not produce urine, it may shrink, a process called atrophy. Once connected to a functioning kidney, the bladder will begin to stretch until it is able to function normally. This happens over a period of time.
19:54:38
Shenoy and the surgical team look for evidence that Emily’s new kidney is functioning properly. When that information is confirmed, the last sutures are made, and the kidney transplant is complete.
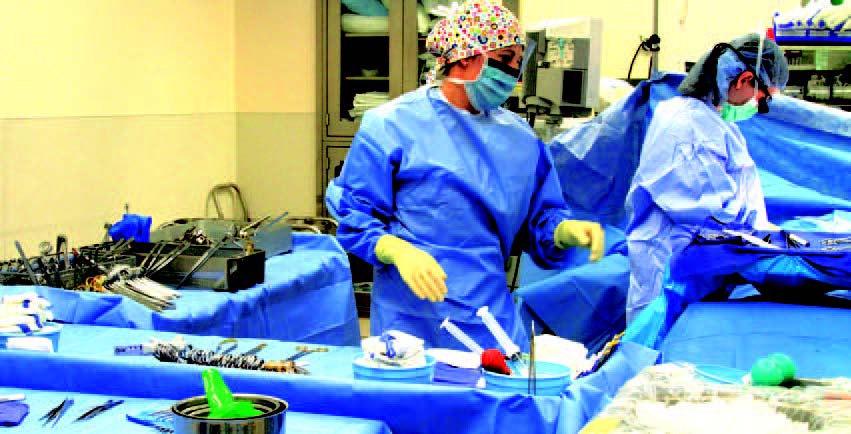
After Surgery
Emily is a patient at Barnes-Jewish for six days following her transplant surgery. Once home, her new kidney’s urine output is closely monitored. Blood is drawn at specified times to monitor the function and efficiency of the new kidney. To ensure against organ rejection, Emily takes medications to suppress her immune system. After recovery, Emily is enjoying life with her husband, family and friends.
“Once the new kidney begins to function normally, the patient can return to a normal life, free of dialysis,” says Shenoy.
Learn more about kidney transplant by visiting BarnesJewish.org/kidneytransplant.
The Living Donor Kidney Transplant Program
Emily received her new kidney from a living donor through a paired-kidney exchange. This novel approach allows patients with kidney failure who have a suitable, but mismatched potential kidney donor to exchange donors. Each donor gives a kidney to a different recipient than he or she originally intended, and each recipient is able to receive a living-donor kidney, rather than remain on the waiting list.
A patient in need of a kidney transplant reaps a number of benefits when the donated kidney comes from a living donor rather than a deceased donor.
Surendra Shenoy, MD, PhD, a Washington University transplant surgeon at Barnes-Jewish Hospital and director of the living-donor transplant program, says, “In general, patients who receive a kidney from a living donor have a better chance of the kidney lasting up to 20 years. A kidney from a deceased donor may last 10 to 12 years.” Patients who receive a kidney from a living donor usually spend less time in the hospital after the surgery and experience fewer complications.
The availability of a living-donor kidney also can ensure a patient doesn’t remain on the waiting list for an extended period of time. The longer the wait-list time, the more diminished a patient’s quality of life becomes.
Wait-list time, which may last as long as five years, can contribute to organ rejection. In addition to cleansing blood by the removal of waste, kidneys also produce erythropoietin, a hormone that stimulates production of red blood cells in the bone marrow. When kidneys fail, transfusions are used to stimulate blood marrow production. “Every transfusion exposes the patient to an antigen that can produce the antibodies that trigger organ rejection. The longer a patient in kidney failure is on the wait list for a kidney, the more sensitized that patient becomes and the greater the risk of organ rejection once a kidney is transplanted,” says Shenoy.
New techniques used to remove a kidney from a living donor have reduced postoperative pain and recovery time.
To learn more about the living-donor kidney transplant program at Barnes-Jewish Hospital, visit BarnesJewish.org/kidneydonor or call 314-TOP-DOCS (314-867-3627) or 866-867-3627 (toll free).