Learning that you have hypertrophic cardiomyopathy can seem overwhelming, but your care is in expert hands with our highly skilled team. At the Hypertrophic Cardiomyopathy Center of Excellence at the Washington University and Barnes-Jewish Heart & Vascular Center, we offer comprehensive care. Using the newest therapies, we can treat everyone with hypertrophic cardiomyopathy, no matter their health needs.
What Is Hypertrophic Cardiomyopathy (HCM)?
Hypertrophic cardiomyopathy (HCM) is a structural heart disease that causes thickening of the heart muscle. The thickening involves the heart muscle of the left ventricle (lower heart chamber) and can occur in different patterns. In most people, HCM typically affects the septum, the muscle wall between the left and right sides of the heart.
The thickened septum can narrow the left ventricle, sometimes blocking blood flow from the heart. This thickening also causes extra stiffness in the heart’s walls. These changes prevent the heart from working properly, forcing it to work harder to pump enough blood to the body.
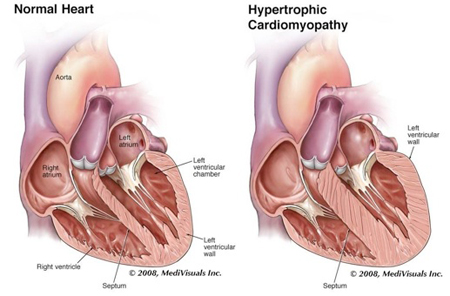 |
| Illustration depicting the difference between a normal heart and hypertrophic cardiomyopathy |
Hypertrophic Cardiomyopathy Center of Excellence in St. Louis
At the Hypertrophic Cardiomyopathy Center, our team has decades of experience treating HCM. People come to us from surrounding states for our:
- Expert team: Our multidisciplinary program includes board-certified specialists in interventional cardiology, cardiac surgery, general cardiology, cardiac imaging, electrophysiology and cardiac genetics. Through advanced fellowship training and collaboration, we have developed expertise in caring for people with the most complex cases of HCM.
- Center of excellence: The Hypertrophic Cardiomyopathy Association has named us as one of only about 40 centers of excellence nationwide, and we are the only HCM center of excellence in the region. Our team provides every aspect of care for people with HCM, including diagnostic testing, up-to-date medical therapies, and advice and genetic testing for family members.
- Advanced diagnostic capabilities: Our diagnostic imaging technicians use state-of-the-art technology to help doctors determine a diagnosis. Our dedicated sonographers have specific training in HCM-focused echocardiograms, and we also have the latest cardiac MRI capabilities.
- Groundbreaking research: For the past few decades, doctors treated HCM with medications originally developed for other heart conditions. Through research, we are pioneering promising new medications designed specifically to treat HCM. Our center is studying improved techniques for diagnosing HCM and conducting clinical trials to advance new and more effective treatments. We are at the forefront of research that may entirely change the landscape of treatment for HCM.
Causes and Risk Factors of Hypertrophic Cardiomyopathy
In most cases, HCM is inherited, and it results from mutations (changes) in genes that control heart muscle growth. Some people who have these genetic changes never develop HCM. But they still may be able to pass the gene mutations on to their children.
Symptoms of Hypertrophic Cardiomyopathy
Some people who have HCM don’t experience symptoms, at least in its early stages. As HCM worsens, you may develop symptoms such as:
- shortness of breath, especially with physical activity
- chest pain or pressure (angina), especially with physical activity
- fatigue (tiredness)
- lightheadedness or fainting
- sensations of rapid, fluttering heartbeat (palpitations) caused by arrhythmias (irregular heart rhythms)
Diagnosing Hypertrophic Cardiomyopathy
To diagnose HCM, we perform a thorough evaluation. This process includes a discussion about your symptoms and personal and family medical history along with a complete physical exam. You may need tests, such as cardiac imaging or genetic testing, to confirm a diagnosis. Learn more about our diagnostic testing for cardiovascular disease.
Because HCM may run in your family, we may recommend that your family members be screened for signs of HCM. Our thorough approach includes referrals for genetic testing and counseling with a geneticist to help guide care decisions for you and your family.
Hypertrophic Cardiomyopathy Treatments
Based on your evaluation results, we work with you to create a comprehensive treatment plan tailored to your needs. Treatment goals are to relieve your symptoms and reduce your risk of complications such as heart failure and sudden cardiac death.
The treatment options for HCM include:
- Medications: Medications can help the heart pump more effectively, control arrhythmias, and help prevent blood clots if you have atrial fibrillation.
- Transcatheter alcohol septal ablation: Our interventional cardiologist performs a minimally invasive (nonsurgical) procedure to thin part of the thickened heart tissue. Through a tiny incision, we insert a catheter (thin, flexible tube) to deliver a small amount of alcohol. We place the alcohol into the thickened septum where it is blocking blood flow from the heart. The alcohol destroys the targeted tissue, which thins the thickened septum and successfully removes the obstruction.
- Septal myectomy: Our cardiac surgeons specialize in this intricate, open-heart procedure which removes a portion of the thickened heart muscle of the septum. For this intricate surgery, it’s crucial to have a highly experienced cardiac surgeon who specializes in the procedure, like those who perform it at Barnes-Jewish Hospital.
- Implantable cardioverter defibrillator (ICD): If you are at risk for arrhythmias or sudden cardiac arrest, an ICD can help reduce that risk. Our electrophysiologist (specialist in the heart’s electrical system) implants ICDs to help maintain a regular heartbeat. We also specialize in using a less-invasive type called a subcutaneous ICD.
Contact Us
To make an appointment with a Washington University cardiovascular specialist at Barnes-Jewish Hospital, please call 888-202-6626.